
How Myofascial Release Therapy Can Improve Occupational Performance
By Rachel Gottesman, OTR
In my seventeen years of practicing occupational therapy, I have seen the impact pain has on clients and their performance of day to day activities. While I have helped people using adaptive equipment, therapeutic exercises and activities, there are times when, despite my best efforts, pain continues to limit a client’s performance in occupational roles. Frustrated, I found myself searching for another modality which could help clients return to their valued roles and activities. That is when I found that fascia can play a significant, yet overlooked role in the body’s function.
The types of patients or clients who may benefit from MFR are:
- Those who have had constant pain which limits their participation in their occupational therapy program.
- It may be the person who fatigues easily or when therapeutic exercises or strengthening are very limited or may exacerbate their pain (for example shoulder arthritis).
- The person who appears disengaged in what you are trying to do in your session (who may keep their eyes closed or demonstrates limited communication).
- Myofascial release also might help the person who is plateauing with traditional strengthening and range of motion techniques.
- The ideal person for myofascial release someone who is motivated to get better but finds it hard to do so secondary to pain or fatigue.
- It is also the person who understands that they must play an active role in their therapy process (versus a “fix me” mentality).
- It is the person who understands the importance of a home exercise program.

Example of a Myofascial Release Technique
Myofascial Release or MFR can complement traditional occupational therapy modalities
MFR techniques can facilitate passive, active and active assisted range of motion in preparation for functional activities. For example, if a client is having shoulder pain which limits their arm use in overhead activities such as hair combing, MFR can help to increase shoulder range of motion so the activity can be done with more ease. This is done by releasing the restrictions that have been locking down the area.
For those with chronic pain, MFR techniques can be effective as well. By using slow sustained pressure at the barrier of a restriction, the fascia starts to change and return back to a fluid, healthy state. Over time even chronic restrictions can start to transform. Once a patient or client experiences a difference in their range of motion or pain levels versus thinking they will just have to live with the pain. They can start to overcome the “hurdle” which had limited their progress with therapies in the past.
A typical OT/MFR session
I initially review the patient’s goals, including what activities in their Activities of Daily Living and routines they feel they are limited. I then explain what myofascial release is, and how it can complement their occupational therapy goals. I also explain what their role in the process will be. Then I perform MFR techniques, starting with their symptoms, but looking elsewhere for the cause. These techniques can be combined with exercises/activities to help facilitate releases. Finally, I review activity modification strategies, home exercise or self-treatment ideas so their bodies can continue to maintain the changes made in the OT session for ease of performance in their ADL and IADL tasks.
I work with patients in a private practice as well as a hospital setting. In the hospital setting I take objective and subjective measurements towards a client’s occupational goals. In as little as a few weeks, clients have reported improvements on the PSFS scale (patient specific functional pain scale which is a subjective measure of their ability to perform an occupational activity), as well as objective improvements with functional reach, upper extremity range of motion, and grip strength.
In the acute care setting
I have seen MFR reduce a patient’s heart rate, blood pressure as well as respiratory rates. Patients have also reported less post-operative pain, especially after spinal surgery. MFR can be used before ADL retraining. I have observed improvements in engagement in activity as well as decreased pain when performing the activity. For example, a patient was able to demonstrate increased external rotation of hip so she could put on her socks without adaptive devices. These techniques can be performed less than 10 minutes thus meeting the expectation for efficient care.
In outpatient practice
Clients learn to help themselves by encouraging them to take an active role in their own therapy process. This can include following through self-treat suggestions between sessions and when necessary, a shift in the way they think about or relate to the experience of pain. By working the physical and mental aspects of treatment, one can experience more freedom in the way their bodies move. They can also adapt more easily by knowing what to do if pain or limitations arise in their day to day activities.
Like every therapy, myofascial release does have a few contraindications
These include acute fractures, brain bleeds, and direct compression on bone metastes. Lack of motivation in the healing process is indicative that one may not benefit from myofascial release therapy.
What is fascia?
Fascia is a web of densely woven connective tissue, covering and interpenetrating every muscle, bone, nerve, artery and vein, as well as all of our internal organs. This includes the heart, lungs, brain and spinal cord. Fascia is actually one continuous structure that extends from head to toe without interruption.
Each part of the entire body is connected to every other part by the fascia, like the yarn in a sweater.
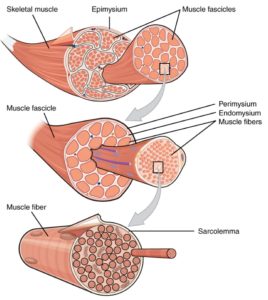
Cross-section of muscle fiber showing fascial tissue between structures. Image courtesy Anatomy and Physiology (OpenStax 2016).
By surrounding every structure in the body, fascia affects these structures at the cellular level, including the transport of nutrition in and out of the cells. Without this proper flow, a body can’t reach optimal function.
Fascial restrictions can be thought of as a “knot” in the facial web. These restrictions can place up to 2000 lbs of tensile force on pain sensitive structures. Fascial restrictions often go undiagnosed because they do not show up on traditional tests (CT, MRI, x-ray).
Restrictions develop for many reasons
This can include physical or emotional stress, poor posture, surgery, trauma, and repetitive stress over time.
Three components to the fascial system:
- Elastic
- Collagen
- Ground Substance

Fascial restrictions resemble the knots in the strands of this fishing net (Image courtesy Oxfordian Kissuth, Wikimedia Commons).
Just stretching the elastic length of the fascia does not produce long lasting changes to the system. For that we need to make changes in the ground substance. The ground substance is solidified when restricted. By providing sustained holds, at least three to five minutes, we start to change the ground substance back to its fluid like state, allowing ease of movement.

Rachel Gottesman has been in practice for over seventeen years. She has been incorporating myofascial release (MFR) into her practice and has performed MFR techniques on clients ranging in age from 3 to 95 years with a wide variety of conditions and diagnoses. Learn more at www.bodyeasetherapy.com
Edited by Emmy Vadnais, OTR/L





Leave a Reply